Stigma, misunderstanding, and weak linkages to our nation’s healthcare system has led to significant disparities in Alzheimer’s and dementia diagnosis rates, access to treatment, quality care, clinical research and trial participation rates among Latinos and African Americans, according to a recent study published by the Alzheimer’s Association.
The study examined annual statistics and interview data from over 2,500 Americans who currently or recently were caregivers of adults age 50 or older with cognitive issues. The respondents included just over 1800 Black, Indigenous, and People of Color (BIPOC). The study reiterated that many non-White Americans experience discrimination in the broader health care system.
Webinars on Racial Differences in Dementia Care
Addressing Systemic Racism: The Impact on African Americans with Alzheimer’s Disease and Related Dementia, University of Wisconsin. Madison, June 2020.
Racial Disparities and Their Impact on Incidences of Dementia and Barriers to Caregiving, Alzheimer’s Foundation of America, August 2020.
Viewing the above webinars does count towards the dementia care training requirement outlined in NH RSA 151:48-51. Track your own progress with the Participant Training Tracker as .xls.
Findings from the Special Report concluded 66 percent of Black Americans believe it would be hard for them to get what they perceive as “excellent” care for the dementia. Nearly 40 percent of Native Americans, 39 percent of Hispanics, and 34 percent of Asian Americans shared that view. All were also likely to distrust medical research and unlikely to believe health care professionals empathize with them.
This study is all the more alarming because black Americans are twice as likely to develop Alzheimer’s disease, and Hispanic/Latinx one and a half times more likely, than their white counterparts. Studies are now exploring the risk factors which may contribute to these findings, including healthcare disparities and race-based traumatic stress.
“Discrimination, lack of diversity among health care professionals, and mistrust in medical research create significant barriers to care and demand the country’s full attention,” Carl V. Hill, Ph.D., MPH, chief diversity, equity and inclusion officer of the Alzheimer’s Association, said in a statement.
Other key findings from the report include:
- People of color want health providers who understand their unique experiences and backgrounds, but many doubt they would have access to culturally competent providers.
- Black Americans lack trust in research trials and half doubt that their community will share in treatment advances.
- Knowledge, awareness, concern, and stigma about Alzheimer’s vary widely across racial and ethnic groups.
These findings are significant as recent studies indicate older black Americans are nearly twice as likely to have dementia than older white Americans.
Black Americans were twice as likely as other groups to say they “don’t trust medical research” and more than twice as likely to say they “might not be treated fairly.” Notably, the survey found that 36% of black Americans, 18% of Hispanic Americans, and 19% of Asian Americans felt that discrimination put a barrier on their access to receive care for Alzheimer’s disease. In total, 42% of Native Americans, 34% of Asian Americans, and 33% of Hispanic Americans reported having experienced discrimination when navigating health care settings for their care recipient. For black Americans, that rate was 50%.

What race is most affected by Alzheimer’s disease?
Among people ages 65 and older, African Americans have the highest prevalence of Alzheimer’s disease and related dementias (13.8 percent), followed by Hispanics (12.2 percent), and non-Hispanic whites (10.3 percent), American Indian and Alaska Natives (9.1 percent), and Asian and Pacific Islanders (8.4 percent).
According to findings published in JAMA Neurology, rates and incidence of dementia among non-Hispanic black individuals remained substantially higher than non-Hispanic white individuals in the U.S. from 2000 through 2016.
Unfortunately, black Americans and other racial minorities are severely underrepresented in studies and clinical trials regarding diagnosis and treatment.
“In the U.S., multiple studies report that the risk of dementia is higher in non-Hispanic black individuals than in non-Hispanic white individuals,” the researchers wrote. “These disparities mirror those in other health domains, which are broadly attributed to the cumulative effects of structural racism; likewise, structural racism may affect brain health through material, behavioral and biological mechanisms.”
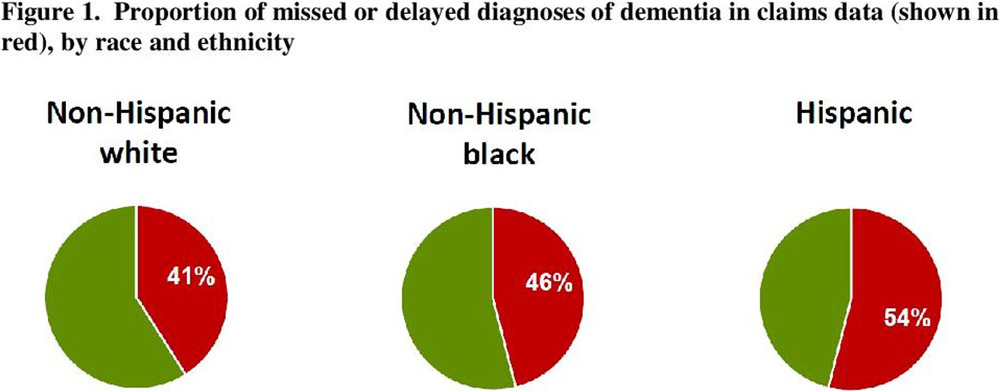
https://doi.org/10.1002/alz.043183
Race and Ethnicity Impact Alzheimer’s Care, Perceptions
Findings from nationwide surveys of Asian, Black, Hispanic, Native, and white Americans — conducted with U.S. adults and Alzheimer’s caregivers — reveal compelling insights into how these groups view Alzheimer’s disease, medical research, and barriers they face accessing dementia care
Regardless of race or ethnicity, survey respondents see affordability as the most likely barrier to excellent care and support for Alzheimer’s or dementia — ranging from 70 percent of Asians to 52 percent of Blacks. To a lesser extent, Americans also see a lack of health insurance coverage, services missing in their community, and a lack of family and community support as likely barriers.

Racial Disparity Not Improving
According to Melinda C. Power, ScD, associate professor in the department of epidemiology at George Washington University’s School of Public Health, and colleagues, the National Alzheimer Project aims to reduce these disparities in Alzheimer’s disease among racial and ethnic minorities at greater risk for the disease. She maintains it is essential to track racial and ethnic disparities to determine what progress has been made.
Their study found that non-Hispanic black participants experienced an approximately 1.5 to 1.9 times greater prevalence of dementia across all algorithms than with non-Hispanic white participants in all waves from 2000 to 2016 in both crude and standardized estimates. Overall rates of dementia decreased with time, but relative rates of dementia across non-Hispanic black and non-Hispanic white participants did not change significantly over time. Standardization for age and sex revealed no evidence of a declining racial disparity over time.
“Additional efforts to identify and mitigate factors contributing to these disparities is warranted,” wrote Power and colleagues. “Efforts to improve our capability to quantify and track dementia risk overall and by key sociodemographic groups are also needed. Such efforts would improve our ability to target interventions and track progress toward reducing both overall dementia risk and disparities in dementia risk.”
More on Alzheimer’s Disease Racial Disparity
Babulal, Ganesh M, et al. “Perspectives on Ethnic and Racial Disparities in Alzheimer’s Disease and Related Dementias: Update and Areas of Immediate Need.” Alzheimer’s & Dementia : the Journal of the Alzheimer’s Association, U.S. National Library of Medicine, Feb. 2019, www.ncbi.nlm.nih.gov/pmc/articles/PMC6368893/.
Chin, Alexander L, et al. “Diversity and Disparity in Dementia: the Impact of Ethnoracial Differences in Alzheimer Disease.” Alzheimer Disease and Associated Disorders, U.S. National Library of Medicine, 2011, www.ncbi.nlm.nih.gov/pmc/articles/PMC3396146/.
Fairley, Acanthus. “Aging Through Traumatic Stress: Analyzing the Effects of Traumatic Stress and Race on Alzheimer’s Disease.” Alzheimer’s Foundation of America, Alzheimer’s Foundation of America, 28 July 2020, 5:30 pm, alzfdn.org/event/webinar-aging-traumatic-stress-analyzing-effects-traumatic-stress-race-alzheimers-disease/.
Green-Harris, Gina, et al. “Addressing Disparities in Alzheimer’s Disease and African-American Participation in Research: An Asset-Based Community Development Approach.” Frontiers, Frontiers, 13 May 2019, www.frontiersin.org/articles/10.3389/fnagi.2019.00125/full.
“Injury Center.” Centers for Disease Control and Prevention, Centers for Disease Control and Prevention, 8 Dec. 2020, www.cdc.gov/ncipc/duip/fallsmaterial.htm.
“Injury Center.” Centers for Disease Control and Prevention, Centers for Disease Control and Prevention, 8 Dec. 2020, www.cdc.gov/ncipc/duip/fallsmaterial.htm.
Lin, Pei-Jung, et al. “Dementia Diagnosis Disparities by Race and Ethnicity.” Alzheimer’s Association, John Wiley & Sons, Ltd, 7 Dec. 2020, alz-journals.onlinelibrary.wiley.com/doi/full/10.1002/alz.043183.
“Materials for Healthcare Providers.” Centers for Disease Control and Prevention, Centers for Disease Control and Prevention, 12 Aug. 2020, www.cdc.gov/steadi/materials.html.
Urban, Peter. “How Race and Ethnicity Impact Alzheimer’s Disease Care.” AARP, 5 Mar. 2021, www.aarp.org/health/dementia/info-2021/health-disparities-alzheimers.html.

